Spinal stenosis is common and can happen anywhere in the spine but it is most common in the lumbar spine (low back) and the cervical spine (the neck) because these are the most mobile parts of the spine.
Narrowing of the spinal canal can result in abnormal pressure on the spinal cord and spinal nerves.
Spinal Stenosis
Spinal stenosis is most commonly due to degenerative changes in the spine or “wear and tear” and is part of the natural ageing process. Wear and tear can affect different parts of the spine which causes a narrowing of the spinal canal and compresses the spinal nerves and spinal cord. The result is a debilitating condition that limits a person’s ability to walk, exercise and enjoy many other activities which reduces their quality of life.
The narrowing of the spinal canal is predominantly due to degenerate discs, enlarged facet joints, bony spurs and thickening of the longitudinal ligament (one of the ligaments that supports the vertebral column).
If the there is a central disc bulge, it may be described as a ‘Central Canal Stenosis’. However, if the disc bulge is more to one side or another in combination with enlarged facet joints and ligaments there maybe ‘Foraminal Stenosis’ or ‘Lateral Recess Stenosis’ on the left, right or bilaterally. For you it does not really matter however you may hear these descriptions as part of your diagnosis. They relate specifically to where the narrowing is and affect how the surgery will be approached.
Symptoms include:
- Pain in the legs or arms (there may or may not be pain in the back/neck)
- Loss, altered or ‘numbness’ sensation
- Burning
- Pins and needles/tingling
- Weakness, jelly or heavy sensation in the arms or legs
- Myelopathy
- Loss of bowel, bladder or sexual sensation/function – this is rare and is called Cauda Equina Syndrome and you should seek urgent medical attention.

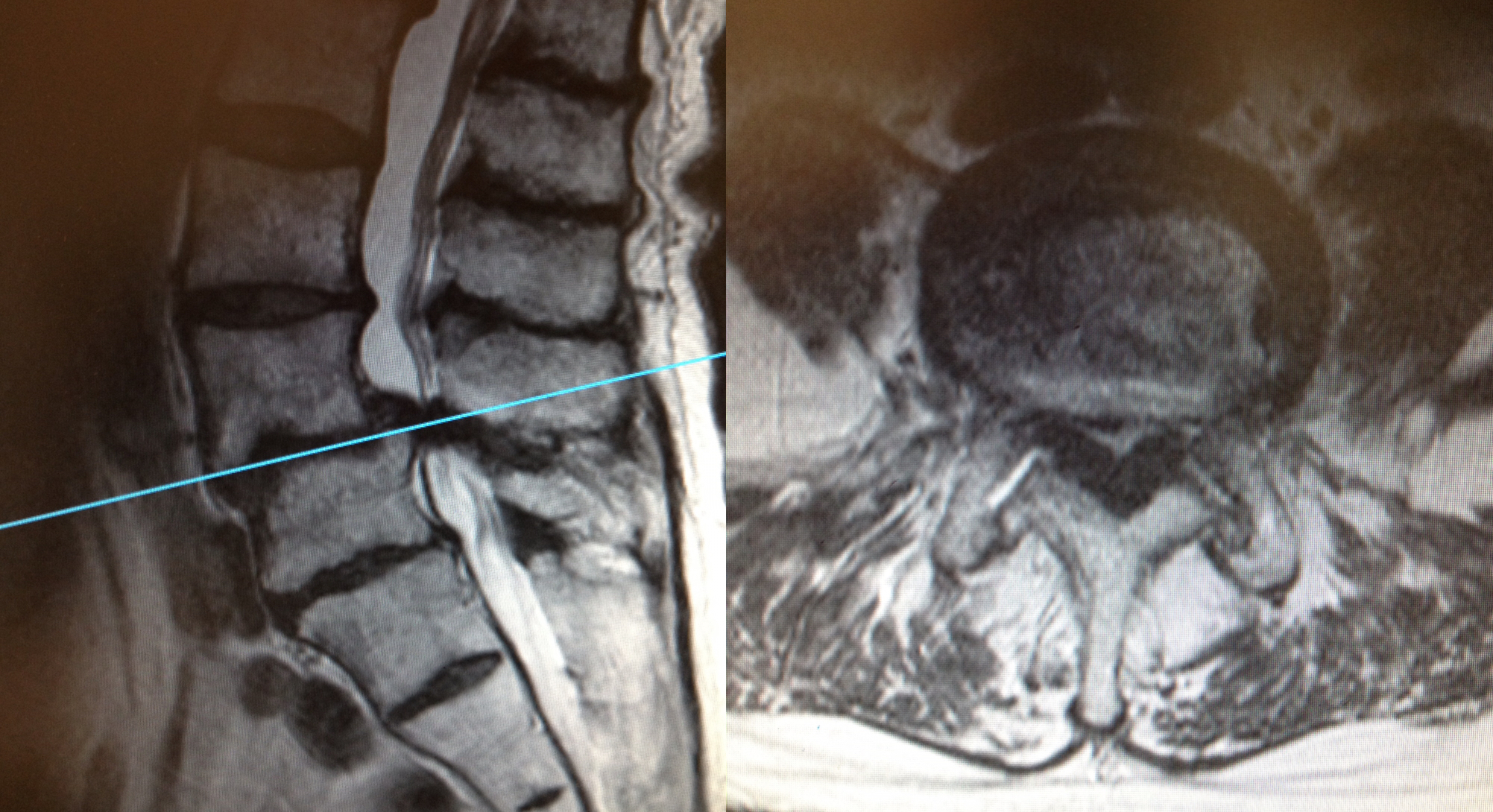
The MRI scans show severe spinal stenosis at L4/5 caused by a degenerative disc, longitudinal ligament and facet joints and the stenosis has been made worse by a degenerative spondylolisthesis (anterolisthesis) at L4/5.
Lumbar Decompression
All lumbar decompressions are performed in theatre under a general anaesthetic and typically most patients stay in hospital for 1 – 2 days.
Mr Hilton performs all decompressions and discectomies under X-ray guidance (to confirm the correct level) and with the use of a surgical microscope – this allows an excellent, magnified view of the whole of the surgical area. In a decompression only the bulging part of the disc, the bony spurs and enlarged part of the ligament is removed to create space around the nerves and to allow the free flow of CSF.
The whole operation is performed through a small incision which is about 3cm long, however it maybe longer especially if the operation involves more than one level.
The first part of the operation is gaining access to the spinal canal which involves removing a small amount of bone and ligament. The irritated nerve root lies on top of the disc that is being operated on, therefore the nerve has to be carefully moved and protected (‘retracted’) for the next part of the operation.
Often nerves that have been compressed or irritated can be ‘stuck’ down onto the disc and so it can be quite difficult to simply move the nerve out of the way. Once the nerve is moved out of the way and protected, the soft tissue and bone material that is causing increased pressure on the nerve is removed.
Risks And Complications Of Decompression
- Bleeding (minor and major vascular damage which can be life-threatening)
- Bruising around the surgical site
- Infection
- DVT/Pulmonary Embolism
- Dural tear/CSF leak (about 8% risk)
- Wound dehiscence
- Minor and major nerve damage (including foot drop, cauda equina syndrome, paralysis) which can be temporary or permanent
- Damage to surrounding soft tissues including muscle
- Perineural fibrosis (scarring around nerves)
- Failure to relieve symptoms, recurrence or worse symptoms
- Back pain
- Medical complications including stroke (CVA), heart attack (MI), blindness and death.
Mr Hilton will take time to thoroughly go through all the risks and complications of a decompression before you decide whether to proceed with the surgery.
More detailed information about the general risks and complications please look at the ‘Risks and Complications’ section.
Recovery
Everybody is different! Initially when pressure is taken off a nerve most patients immediately feel pain relief whereas for others it can take a few days. This is because nerves that are inflamed take time to settle and surgery itself can cause some temporary inflammation of nerves.
The main aim of a decompression is to take the pressure off and create space for the nerves and therefore stop pain and prevent any further loss of power or progressive numbness. The procedure is predominantly performed to relieve pain and for most patients, their pain improves.
It is very difficult to predict whether altered sensation or numbness will improve and unfortunately, for some people, it does not improve despite a good operation. It takes longer for muscle power to improve and this may never fully recover. If there has been any muscle wasting (loss of muscle bulk) this often never returns even if the strength improves.
After surgery it is not uncommon to have various aches and pains in and around the wound, and in the bony pelvis, hips and thighs. These usually improve with time.
Following surgery, most patients usually stay in hospital for 1 – 2 days and this partly depends on their general health. Some pain/tenderness and bruising is normal around the operation site and usually patients feel this is different in nature to the back pain they were experiencing before the operation and improves as the healing process continues.
Prior to your discharge, you will spend time with the hospital physiotherapist who will help you to mobilise (with crutches if needed) and they will advise you on appropriate exercises to do once you return home. It is essential you practice these exercises everyday.
Mr Hilton or one of his team will see you at about 7 – 10 days following your operation to check your wound and also to see how you are getting on. All patients are advised NOT to change their dressings. You are at risk of getting a wound infection if you change your own dressing.
If you are concerned about your wound or you feel it is necessary to change the dressing before your wound check appointment, then either:
Place a fresh dressing over the top of the original dressing
OR
Contact the hospital or your GP practice.
Depending on your job, most patients are able to return to work 6 weeks after the surgery.
Physiotherapy
The first part of your treatment is to take the pressure off the affected spinal nerve, the second part of your treatment journey is your rehabilitation which involves exercise. You will be referred to a physiotherapist as an outpatient, however before you see the physiotherapist please continue to do the exercises you were taught in hospital on a daily basis.
The aim of doing exercises is to rehabilitate and improve the strength of the muscles supporting the spine and pelvis.


